谁生谁死?这是医生面临的痛苦抉择
The heart-wrenching choice of who lives and dies
By Abigail Beall
Shortages of equipment, beds and staff means doctors have a dreadful decision to make in the midst of the current pandemic.
There is something strangely quiet about the wards of coronavirus patients in Lodi, Italy. Even though the hospital corridors bustle with medical staff, the patients make little noise, says Stefano Di Bartolomeo. For a doctor experienced in working in conflict situations, this pandemic has felt unusual.
“Everybody has their own little bag with personal belongings on the ground or hanging from their trolleys,” says Di Bartolomeo, an anaesthetist working at a hospital in Lodi. Nobody is allowed visits from their family members, so their phones are the only line of communication. Many patients, although critically ill, do not feel they are that bad, and some don’t even notice trouble breathing.
Perhaps most unusually of all, even though many require a bed in intensive care, they won’t all get put into one. When a bed in intensive care does become free, the doctors must decide which patient it will be given to.
Di Bartolomeo, who has a background in tropical medicine and epidemiology, began at the Lodi hospital in mid-March as part of a mission with Médecins Sans Frontières. It was a shock: cases there had already reached 1,100 by 13 March. “The hospital has been coping with the situation, but at the same time [it’s] completely overwhelmed,” he says.
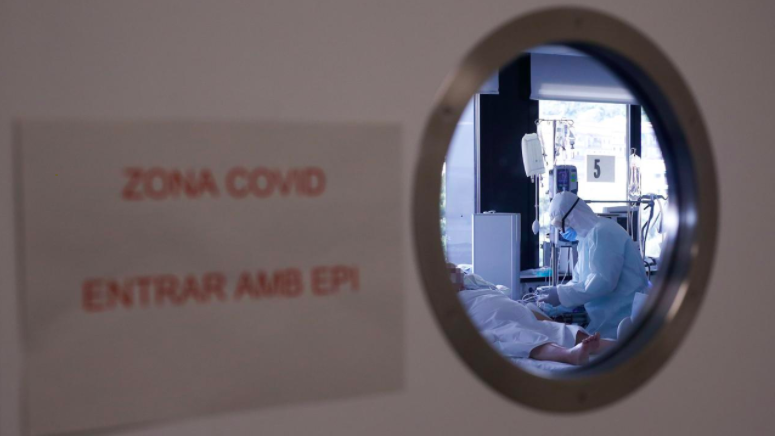 Much of the equipment needed to treat Covid-19 patients is in limited supply, forcing doctors to decide who gets it (Credit: Getty Images)
Much of the equipment needed to treat Covid-19 patients is in limited supply, forcing doctors to decide who gets it (Credit: Getty Images)
Di Bartolomeo is currently working on a ward where patients are given non-invasive ventilation while they wait for a bed to become available in intensive care, where they can be intubated with a tube placed into their airways through their mouth. But not all patients are put through to his ward. “Some patients, because they are too old or too sick, they are just put on oxygen,” Di Bartolomeo says. “They are not candidates for other forms of more invasive support like CPAP (continuous positive airway pressure) or non-invasive ventilation.”
Difficult decisions
As the number of people who have tested positive for coronavirus around the world exceeds three million this week, the virus is stretching health services to breaking point. As of 28 April, more than 212,000 people have been confirmed to have died with the virus. In hospitals across many of the 210 countries to have been hit by the pandemic, beds are filling up with Covid-19 patients.
In some cases, important resources like ventilators, protective equipment and even medical staff are becoming scarce. Doctors are being forced to make a choice of who to prioritise caring for.
But how can anyone put more value on one life over another – never mind someone who has sworn to “do no harm”?
Medical groups have tried, although their resulting guidelines – and the logic behind them – have come under strong criticism.
How can anyone put more value on one life over another – never mind someone who has sworn to “do no harm”?
On 23 March 2020, a group of doctors and academics from around the world published a set of ethical guidelines in the New England Journal of Medicine (NEJM), outlining how to ration resources during the Covid-19 pandemic. Among the recommendations made by the paper’s authors is that at times like this, the usual approach of treating people on a “first-come, first-served” basis should not apply. It also urges prioritising severely ill patients who are younger and who have fewer existing health conditions.
This echoes guidelines given to Italian doctors, which say they may need to prioritise those who will have the greatest chance of successful treatment. Published on 6 March 2020, the Italian guidelines compared the circumstances doctors and nurses are working under to “catastrophe medicine” and stated that it “may be necessary” to place an age limit on those being admitted to intensive care.
“The top consideration is maximising benefits in terms of the number of lives saved and the number of life years saved,” says Ezekiel Emanuel, chair of the Department of Medical Ethics and Health Policy at the University of Pennsylvania and co-author of the paper.
 For some health care workers, the emotional turmoil of the pandemic could have lasting effects (Credit: Getty Images)
For some health care workers, the emotional turmoil of the pandemic could have lasting effects (Credit: Getty Images)
The argument is that younger, healthier people have a much greater chance of survival, and also a greater life expectancy. Diverting scant resources to these people delivers benefits to the largest number of people, is how the theory goes.
But even for those who accept that logic, it isn’t watertight: the implication, for example, is that both a young person and an old person each on ventilators have the same mortality risk when left unaided, and that a young person taken off a ventilator wouldn’t be more likely to survive than the older person.
The NEJM paper also urges giving groups of people who provide the most value in fighting the pandemic – such as frontline healthcare workers and others who keep key infrastructure going – priority access to medical equipment and treatment on the basis that their jobs require significant training and so they are difficult to replace.
“Because maximizing benefits is paramount in a pandemic, we believe that removing a patient from a ventilator or an ICU bed to provide it to others in need is also justifiable and that patients should be made aware of this possibility at admission,” the researchers write.
Ethical issues
These sorts of decisions are only ever likely to be necessary when hospitals and health care systems are under the most extreme pressure, when cases are at their highest and resources stretched to breaking point.
But de-prioritising vulnerable parts of the population – those who are older or who have pre-existing health conditions – obviously raises serious ethical questions.
That’s all the more true because these populations may be even more vulnerable not only to dying from Covid-19, but from getting infected to begin with. People whose health conditions mean that they require the support of others to eat, dress and bathe, for example, are less able to socially distance.
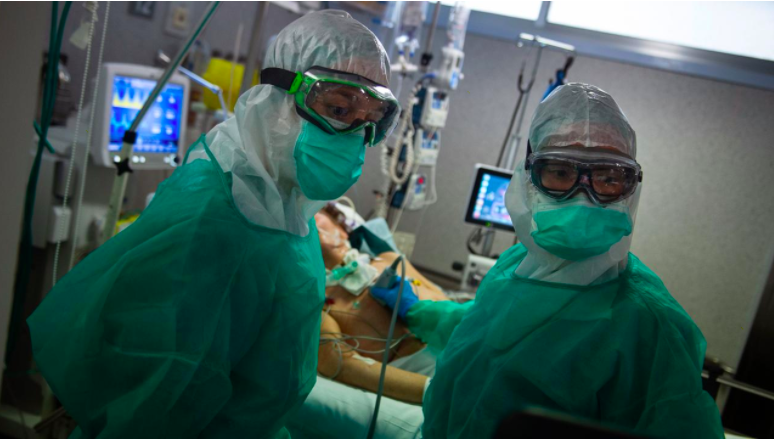 The protective equipment that medical staff have to wear can make the whole experience more frightening for Covid-19 patients (Credit: Getty Images)
The protective equipment that medical staff have to wear can make the whole experience more frightening for Covid-19 patients (Credit: Getty Images)
Meanwhile, the disease has spread quickly around the world through hundreds of nursing and care homes – with devastating results. In England and Wales, a third of all coronavirus deaths have been in care homes, with 2,000 deaths in a single week, for example. Similarly disproportionate numbers have been seen across Europe and in the US, where one-quarter of Covid-19 deaths have been in nursing homes.
Many organisations that support older people are concerned.
"For many years we have known that chronological age is a very poor proxy for an individual’s health status and resilience – something we all see among the older people in our lives," say the heads of a number of British age-related charities including Age UK in a joint statement. "The fact that someone is in need of care and support, in a care home or their own home, should not be used as a proxy for their health status, nor blanket policies applied – for example, over whether they should be admitted to hospital."
An open letter to the British Medical Association, co-signed by that charity Disability Rights UK, also raised concerns that the rights of disabled people are not being upheld.
“Our individual chance of benefiting from treatment should we have Covid-19 must not be influenced by how our lives are valued by society,” the letter says. In response, NHS England insisted that it was seeking to “fully protect the rights of people with disabilities” throughout the course of the pandemic.
Disability groups in the US have also warned against the “deadly form of discrimination” facing people with disabilities during the pandemic
But many of the countries hit hardest by the coronavirus have found themselves having to ask their doctors to make difficult choices about who to prioritise. And those choices are not always based on clear-cut evidence.
In the US, for example, some states already had guidelines in place to address potential ventilator shortages prior to the pandemic. A report in the New York Times examined the publicly available guidelines, from Alabama, Arizona, Kansas, Louisiana, Maryland, Michigan, New York, Pennsylvania, Tennessee, Utah and Washington State, to see how they varied in their definition of who to prioritise for treatment.
In some instances, documents showed that patients with neurological impairments, dementia or Aids might be excluded from receiving ventilator support in some states. Alabama’s plan wrote that those with “severe mental retardation, advanced dementia or severe traumatic brain injury may be poor candidates for ventilator support”, yet went on in the next sentence to add that “the average life expectancy of persons with mental retardation now spans to the seventh decade and persons with significant neurological impairments can enjoy productive happy lives.” The decade-old Alabama plan has since been replaced with another set of guidelines following a challenge lodged by US disability rights groups. The new guidelines, however, do not tackle how physicians should prioritise ventilator triage at all.
Disability groups in the US have also warned against the “deadly form of discrimination” facing people with disabilities during the pandemic. "Every life is valuable," says Neil Romano, chairman of the National Council on Disability. "In this unprecedented crisis, it is crucial that each state respond to Covid-19, not only by supporting its medical professionals' abilities to treat, but by committing to protect the civil rights of its residents with disabilities."
Paola Barbarino, chief executive of Alzheimer's Disease International, says that they have been hearing from their member organisations around the world about decisions to limit treatment based on age and underlying health conditions.
"It is vital that age and conditions like dementia, are not used to discriminate or to withhold access to treatment," she says.
 In many countries, medical staff are being publicly applauded for the work they are doing (Credit: Getty Images)
In many countries, medical staff are being publicly applauded for the work they are doing (Credit: Getty Images)
In the UK, meanwhile, the National Institute for Health and Care Excellence (NICE) issued new guidelines on the 21 March that explain out how to assess whether to intubate patients over 65 without stable long-term disabilities. This is based on a frailty score called the Clinical Frailty Scale, which ranges from 1 to 9, 1 being very fit and 9 being terminally ill. But any assessment, no matter how objectively it’s meant to be done, comes with challenges. The Frailty Scale asks, for example, whether a patient requires help preparing meals or if they have help with stairs – information a physician might not have immediate access to.
One doctor at a London hospital told the BBC just how an assessment like the Frailty Scale can fail. After being asked how far she could walk without having to stop to catch her breath, one patient was deemed as being unfit for a ventilator. But when doctors phoned her family they obtained further information that suggested she might not be as frail as the triage assessment suggested – it turned out the patient had been answering the questions according to her current condition rather than how she was normally. The patient intubated later that day.
The British Medical Association has also issued an ethics guidance document on 1 April stating “health professionals may be obliged to withdraw treatment from some patients to enable treatment of other patients with a higher survival probability.” In some cases, it says, this could mean taking away treatment for someone who is stable or even improving, in favour of another patient with a more positive prognosis.
All across the world, hospitals and health authorities are issuing similar guidelines to help their medical staff make the difficult decisions they are now facing. They are being put in place to try to save people. But they not only affect the physical health of people who are likely to lose out, but also increase their anxiety about what would happen if they do fall ill.
Some doctors have had to take sick leave, feeling unable to face these decisions
There also are concerns about the toll these decisions might take on the mental health of medical staff. For example, some GPs have been taking part in almost daily conference calls to support each other.
People train for years to become doctors because they want to help people in need. The decision to provide care for some patients and not for others is not one any doctor wants to make. Some doctors have had to take sick leave, feeling unable to face these decisions, according to some doctors who spoke to BBC Future.
Of course, deciding who is worth treating and who cannot be saved is not new – battlefield medics and surgeons regularly have to make those kinds of choices. But knowing that doesn’t make it any easier. One consequence, says Elton, is that mental health care for medical professionals may be prioritised more in future.
“I don't want to underestimate the challenge,” says Elton. “But I think that there may be some examples of excellent practice, which could lead to some really good changes in how we support and look after our medical workforce.”
Perhaps by forcing a discussion about the value we place on human life, it may also lead to improvements in how society’s most vulnerable people can be protected.